Infections through Negligence
Infections which are poorly managed or misdiagnosed, can manifest into life-threatening conditions. If you have suffered harm as a result of a post operative infection or you believe your care was poorly handled which caused you to suffer further injury, you are likely to have grounds for a medical negligence claim.
Surgical procedures inherently involve various risks, with the potential development of infection being one of the foremost concerns. Timely recognition and treatment of postoperative infections are crucial to prevent further health complications. This necessitates diligence and consistent follow-up, including educating patients about signs and symptoms for prompt diagnosis.
Types of Claims for Infection- Related Negligence include:
- Misdiagnosis
- Failure to follow up or monitor infection
- Hospital acquired infections
- Inadequate treatment of infection
- Surgical site/ incision infections
- Failure to follow correct infection control procedures and guidelines
- Failure to provide appropriate prophylaxis post-surgery
Consequences of poorly managed infection:
Poorly managed infections can lead to consequences such as hospital admission for intravenous fluids and antibiotics, necrotic (dead) tissue requiring surgical debridement, and the risk of sepsis—a life-threatening condition.
What is sepsis?
Sepsis occurs when the body’s immune response to an infection triggers an inflammatory reaction, causing organ dysfunction. If not diagnosed and treated promptly, sepsis can progress to septic shock, organ failure, and even death. Negligence claims arise when there is a failure to diagnose and treat sepsis in its early stages.[1]
Hospital acquired infections
Hospitals and operative theatres are expected to be clean and sterile, especially in surgical procedures when a patient’s internal organs are exposed. However, sometimes hospitals are a breeding ground for bacteria which leaves patients vulnerable. Hospital acquired infections can spread by; bacteria on surgical equipment and tools, unclean surfaces bed linen, uncleaned surgical wounds, or transmission through hospital staff.
Two common infections after surgery include:
MRSA
MRSA is a type of staph infection that is resistant to many standard typesof antibiotics, giving it the name as a ‘superbug’.It often presents as small reb bumps but can quickly turn into significant, painful abscesses. Left untreated, MRSA can cause life threatening infections in bones, joints, the bloodstream, and lungs.[2]
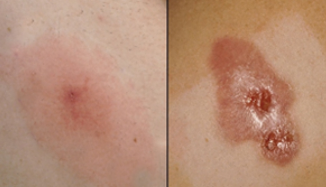
Streptococcus
Streptococcus is a bacterial infection that can also cause life threatening blood and organ infections, however early detection, and treatment with standard antibiotics is usually successful.
Medical Negligence claims
A common area of litigation occurs for incorrect treatment or diagnosis of post operative infections following hip and knee replacement surgeries.
Common signs of a hip/ knee replacement infection include:
- Swelling or redness at the surgical cite
- Abscess/ drainage from the incision site or wound
- Fever
- Weakness
- Nausea or vomiting
- Pain or stiffness at the surgical site
To diagnose an infection, a medical professional should conduct the relevant tests including; bloods and urine cultures, wound swabs, x ray and MRI for a complete assessment. For a positive infection result, treatment may include intravenous antibiotics, surgical removal of the implant and/ or revision surgery to replace the implant. A defective medical device should also be considered for grounds in a medical negligence claim if it caused you to suffer injury.
To establish a case, your specialised medical negligence solicitor must establish four key elements:
- Duty of care: The medical professional owed you a duty of care.
- Breach: The healthcare provider breached that duty by acting negligently or failing to meet the accepted standard of care
- Causation: The healthcare provider’s breach caused or worsened the hip/ knee replacement infection.
- Damages: Compensation is required because of the knee/ hip infection.
In Old v Miniter [2020], the court found the defendant, an orthopaedic surgeon, had breached his duty of care, for failing to provide sufficient management plans for the plaintiff following an ankle reconstruction surgery where there was risk for infection. However, the plaintiff could not establish a link of factual causation to the osteomyelitis infection which emerged seven years later. The court held that the plaintiff’s infection could not ‘reasonably be said to be due to the fault’ of the defendant and that the infection could have recurred regardless of the defendant’s act, and that no non- speculative reason could be identified. A verdict and judgement were made for the defendant and the plaintiff failed to establish an entitlement for a damages award.
The case of Old v Miniter [2020] exemplifies the complexities involved in proving duty, breach, and causation for a medical negligence claim. It underscores the need for specialized solicitors and medical experts to build a strong case. At Stern Law, our team works alongside highly qualified medical experts to build a strong case to enable you to claim what you deserve.
Reach out to our team at Stern Law, offering a unique and individualised understanding of the sensitive nature of medical negligence claims. We offer empathetic listening and guidance through the complex claims process.
Please call us on (02) 9387 1399 or email us at [email protected]
We look forward to sharing this journey with you.
Disclaimer: The content of this article is intended only to provide a summary and general overview of matters of interest. It does not constitute medical or legal advice and should not be relied on as such.
[1] ‘Sepsis’ Health Direct
[2] Mayo clinic ‘MRSA infection’

